Disucss about the Female stress urinary incontinence.
Female stress urinary incontinence (UI) is a common symptom experienced by significant numbers of adult women. The concern has drawn the significant attention of the healthcare sectors worldwide due to the continuously ageing population. The present essay is an evidence-based discussion on the nursing topic of female stress urinary incontinence (UI). The essay provides a definition of stress UI and the prevalence of the same in Australia. Next, it assesses the financial impact of stress UI on a client. Pathophysiology of the disease, risk factors and complications, and impact of stress UI on psychological wellbeing and intimate relationships with the client are next discussed. The following part of the essay focuses on the recommended referrals, including services available in the area of Brimbank Council. Further, treatment of stress UI would be highlighted with special reference to Australia. Lastly, the role of community nurses in managing and supporting clients with stress UI would be outlined.
Wood and Anger (2014) provided the definition for stress UI as a clinical sign, a urodynamic observation and a symptom involving involuntary leakage of urine on efforts such as coughing, sneezing and exertion. It is an involuntary loss of urine and is so severe that it is known to have adverse hygiene and social consequences. Stress UI in females is a health concern leading to distress and inconvenience in a significant section of the women population around the globe. Though it is common among women of older age, problems with urinary bladder are not always a consequence of age and limited to the elderly population.
Stress UI has effected millions of women across the globe that leads to poor quality of life in those who suffer from it. Urinary incontinence is becoming a high burden of suffering in Australia, and statistics had been gathered by healthcare departments to support this. The Australian Bureau of Statistics Survey of Disability, Ageing and Carers highlighted the prevalence of stress UI in their report published in the year 2012, that indicated that about 1.8% people in Australia suffer incontinence. This finding is determined by the need for assistance with bladder or bowel control and the use of aids. There has been an increase in the rate of this condition by 24% between 2009 and 2012. While 13% of Australian men suffer from stress UI, 37% of women in the country suffer from this condition (aihw.gov.au, 2016). As per the reports of Continence Foundation of Australia (2017), almost 4.2 million people in Australia were living with urinary incontinence in the year 2010. Further estimates were made than the number would increase to 5.6 million by the year 2030. On the basis of such data, it can be rightly said that stress UI have had, and would have in future, a drastic impact on the lives of women in the country.
While the impact of female stress UI on quality of life of sufferers draw special attention in research, the financial impact of the condition for the patient is also worth mentioning. The noteworthy financial loss relates to the high cost of healthcare services accessed to treat the condition. The overall costs for diagnosis, treatment and aftercare are often high, placing patients in a financially draining situation. A detailed view of the financial impact of stress UI had been given by Continence Foundation of Australia (2017) that pointed out that almost $271 million was spent in the year 2010 in Australia for stress UI. Sinclair and Ramsay (2011) had opined that UI is common among women who are employed, and thus the potential impact on employment and working life draws much attention. Symptoms of the condition cause loss of ability to concentrate on work, loss of ability to carry out physical tasks and increased number of breaks. As a result, most of these women remain absent from work for a considerable amount of time and are bound to suffer financial loss.
The pathophysiology of stress UI can be well understood by reading the research paper of Arshiya et al., (2015). The continence pathophysiology has the underlying mechanism involving a series of muscles, nerves, and connective tissue that play a role in dynamically influencing bladder control. The organised arrangement allows complete and timely bladder emptying, and the individual is able to maintain continence when there is abdominal pressure. Continence depends on the lower urinary tract which has to be functionally and structurally normal. Stress UI is the condition occurring when there is considerable damage suffered in the nerves, connective tissue and nerves of the pelvic floor. The main determinants of continence are a function of the urethral muscle, vesical neck function, and urethral support. The action of the levator ani muscles supports the urethra through the connection built with the endopelvic fascia of the anterior vaginal wall. When there is damage suffered in this connection between the muscle and fascia, nerve supply to the muscle is lost. There are also high chances of suffering direct muscle damage. This condition results in incontinence. Further, impairment of vesical neck closure leads to incontinence even when the urethral support is normal. It is to be remembered that the main causes of damage suffered are linked to hyperglycemia, obesity, chronic bacterial colonization and urinary tract infections.
Bagnola et al., (2017) outlined the risk factors for stress UI in their research paper that linked childbirth menopause and pregnancy with UI as the major risk factors. Some of the other risk factors for UI can be attributed to problems of constipation, underlying musculoskeletal or neurological conditions and impaired mobility. The common underlying conditions are arthritis, dementia and stroke. Further, lifestyle and health issues such as cardiovascular disease, diabetes, obesity, developmental disorders, physical inactivity, and poor nutrition, are noted as risk factors for developing stress UI. Certain medications have also bene reported to trigger stress UI. These include certain groups of sedatives, diuretics, many anticholinergic agents and psychopharmaceuticals, that further worsen incontinence. Lavelle and Zyczynski (2016) added age, route of delivery, smoking, and ethnic heritage as the other notable risk factors for UI. Smoking has a striking causal relationship with stress UI since the illnesses related to smoking are the main cause of increased coughing. However, further research is needed to understand how the route of delivery can critically serve as a risk factor for UI in women. The particular changes for stress UI associated with ageing have not been cleary defined, as compared to urge UI.
For most of the patients suffering from stress UI, the condition is a severe chronic one that needs continence aids and personal assistance for managing the condition. Therefore, the stress UI has an adverse impact on the physical as well as the emotional health of the person, placing demands on informal carers and the healthcare system. People have the tendency of perceiving incontinence as an untreatable result of age and life events and are at risk of experiencing depression, reduced quality of life and shame due to this (Opara & Czerwi?ska-Opara, 2014). A little less than one-third of the patients suffering from incontinence consider seeking medical attention for the condition they suffer from. Beyar and Groutz (2017) in this regard had stated that the primary impact of stress UI on the lives of women arises from the anxiety and fear experienced in relation to becoming incontinent in public places. As a result, patients suffer recreational and social withdrawal to a great extent. A large pool of evidence highlight that on the emotional front, women develop feelings of humiliation and stigma. The impact on social relationships deserves special mention since there are high chances of reduced affection, intimacy and physical proximity among partners. The amount and quality of sleep are often hampered as women might need to be awake at night for addressing incontinence. Lastly, elderly women are at risk of suffering falls due to their condition.
The Health Department of Australia has increased service provision in the last few years to address the increasing concern of female stress UI in the country. The different municipalities of almost all major cities of Australia are now equipped with service referrals that patients can access as per their convenience. Brimbank City Council is a local council in Melbourne where patients are referred to the Western Continence Service for accessing healthcare services for stress UI (westernhealth.org.au, 2017). The Western Continence Service is well known for the services offered in connection with assessment and management of continence issues. Self-management is also permitted by the agency wherever applicable. An efficient team functions to serve those in need, that includes physiotherapists, physicans and nurses. The vast range of services includes continence assessment, bladder ultrasonography, urodynamic investigation and surgical referral. The conservative management strategies that are offered as part of the services include bladder training and counselling on daily management of the condition. The services are available at three locations in the city, namely, Sunshine Hospital, Sunbury Day Hospital and Williamstown Hospital. Any client suffering from stress UI is to be referred to the continence nurse advisor who has extensive training in continence care. The health care professional would be able to assess the condition of the patient and help in developing management plan as per the needs of the patient. The nurse can make referral to the pelvic floor physiotherapist and occupational therapist for further care plan (Sharma et al., 2017).
Treatment options for addressing female stress UI in aim at preventing the involuntary loss of urine from the urethra at the time of increase of intraabdominal pressure occurring during coughing, physical activity and sneezing. The treatment strategies for stress UI can be classified into the following groups; behaviour therapy, devices, and surgery (Swenson et al., 2017). Behaviour therapies, such as pelvic floor muscle exercises, bladder training and lifestyle changes help patients in eliminating or reducing episodes of stress incontinence. In addition, strategies for appropriate fluid consumption are also taught to patients. a number of efficient devices have come into the market that helps in controlling the conditions, such as vaginal pessary and urethral inserts. Surgical interventions for treating the condition aim at supporting the neck of the bladder or improving closure of the sphincter. Surgical options include sling procedure, retropubic colposuspension, injectable bulking agents, and inflatable artificial sphincter (Kobashi et al., 2017).
As highlighted by Sharma et al., (2017) the risks involved with surgical procedures, loss of productivity in convalescence and cost of hospitalisation has compelled surgeons to bring modifications in the techniques used. The goal is to bring improvements in safety, efficacy and cost-effectiveness, and effectively minimise invasiveness. As no particular intervention or procedure is optimal in case of all patients, there is a need of tailoring the therapy as per the need of the patient. The way of achieving optimal outcome can be linked with proper diagnosis and selection of the suitable intervention by considering different patient factors (Rovner et al., 2017).
Coming to the next section of the paper, the role of nurses in managing and supporting clients with stress UI is to be highlighted. Clients suffering from stress UI are to be explained that UI is not shameful and that the condition is to be fought against bravely. UI is treatable, and this aspect is to be primarily integrated into patient education. Nurses must place themselves to act as a source of help and information (Moorhead et al. 2014). Patient education must be individualised, and nurses must show sympathy and affection while caring for the patients. Since the impact on the psychological thought process of the clients is distinct, counselling is the best way to address the situation. The rationale behind this suggestion is clear. Education promotes effective management and quality of life is thus improved. Reduction of social, psychological and physical limitations is possible with adequate patient education. Lastly, nurses also have the responsibility of developing their skills to learn about therapies and become specialists (Capobianco et al., 2018).
Coming to the end of the essay, it is to be concluded that female stress UI, though not considered as a life-threatening condition, has to be understood as a major cause of poor physical and psychological health of women. The pathophysiology and risk factors of the condition have been well documented. The condition impairs quality of life for patients, causing a disturbance in social relationships and increased psychological distress due to disappointment and awkwardness. Since the prevalence of female stress UI is on the higher side in Australia, there is an urgent need of increasing service provision to address the growing concern. Heath care bodies must come forward to reforms healthcare strategies that can reduce the social and economic burden of female stress UI in the country
References
Arshiya, S., Noor, L., Rangaswamy, A., & Sundari, T. (2015). Etiology, Risk Factors and Pathophysiology of Stress Urinary Incontinence: A Review. International Research Journal Of Biological Sciences, 4(6), 75-82. Link: https://www.isca.in/IJBS/Archive/v4/i6/14.ISCA-IRJBS-2015-041.pdf
Bagnola, E. Pearce, E. & Broome, B. (2017). A Review and Case Study of Urinary Incontinence. Madridge J Nurs, 2(1), 27-31. DOI: 10.18689/mjn.2017-105.
Beyar, N. and Groutz, A., 2017. Pelvic floor muscle training for female stress urinary incontinence: five years outcomes. Neurourology and urodynamics, 36(1), pp.132-135. DOI: 10.1002/nau.22888
Capobianco, G., Madonia, M., Morelli, S., Dessole, F., De Vita, D., Cherchi, P. L., & Dessole, S. (2018). Management of female stress urinary incontinence: A care pathway and update. Maturitas, 109, 32-38. DOI: https://doi.org/10.1016/j.maturitas.2017.12.008
Continence Foundation of Australia. (2017). Prevalence and economic impact of incontinence in Australia: Deloitte Access Economics 2010 · Key statistics , Continence.org.au. Retrieved 20 January2018, from https://www.continence.org.au/pages/prevalence-and-economic-impact-of-incontinence-in-australia-deloitte-access-economics-2010.html
Incontinence. (2016). Aihw.gov.au. Retrieved 20 January 2018, from https://www.aihw.gov.au/getmedia/cb57d70d-f3dc-49c8-984c-c21e7200ebdc/ah16-3-16-incontinence.pdf.aspx
Kobashi, K. C., Albo, M. E., Dmochowski, R. R., Ginsberg, D. A., Goldman, H. B., Gomelsky, A., … & Vasavada, S. (2017). Surgical Treatment of Female Stress Urinary Incontinence: AUA/SUFU Guideline. The Journal of Urology. 198(4), 875-883. DOI: 10.1016/j.juro.2017.06.061.
Lavelle, E. S. & Zyczynski, H. M. (2016). Stress Urinary Incontinence. Obstetrics and Gynecology Clinics, 43(1), 45-57. DOI: https://dx.doi.org/10.1016/j.ogc.2015.10.009
Moorhead, S., Johnson, M., Maas, M. L., & Swanson, E. (2014). Nursing Outcomes Classification (NOC)-E-Book: Measurement of Health Outcomes. Elsevier Health Sciences.
Opara, J., & Czerwi?ska-Opara, W. E. (2014). The prevalence of stress urinary incontinence in women studying nursing and related quality of life. Przeglad menopauzalny= Menopause review, 13(1), 32. DOI: 10.5114/pm.2014.41086.
Rovner, E., Jacoby, K., Kalota, S., Snyder, J. A., Cline, K., Robertson, K., … & Zuckerman, J. (2017). Three-month primary efficacy and six-month treatment arm results from the success study of an intravesical balloon to treat female stress urinary incontinence (SUI). European Urology Supplements, 16(3), e1504-e1505.
DOI: https://dx.doi.org/10.1016/S1569-9056(17)30916-8
Sharma, N., Firoozi, F., & Kavaler, E. (2017). Female Stress Urinary Incontinence. In Interpretation of Basic and Advanced Urodynamics (pp. 35-42). Springer International Publishing.
Sinclair, A. J., & Ramsay, I. N. (2011). The psychosocial impact of urinary incontinence in women. The Obstetrician & Gynaecologist, 13(3), 143-148. DOI: 10.1576/toag.13.3.143.27665.
Swenson, C. W., Kolenic, G. E., Trowbridge, E. R., Berger, M. B., Lewicky-Gaupp, C., Margulies, R. U., … & DeLancey, J. O. (2017). Obesity and stress urinary incontinence in women: compromised continence mechanism or excess bladder pressure during cough?. International Urogynecology Journal, 1-9. DOI: 10.1007/s00192-017-3279-6.
Western Health (2017). Western Continence Services, Westernhealth.org.au. Retrieved 20 January 2018, from https://www.westernhealth.org.au/Services/Western_Continence_Services/Pages/default.aspx
Wood, L. N. & Anger, J. T. (2014). Urinary incontinence in women. Bmj, 349(15), 4531-4542.DOI: 10.1136/bmj.g453
Essay Writing Service Features
Our Experience
No matter how complex your assignment is, we can find the right professional for your specific task. Contact Essay is an essay writing company that hires only the smartest minds to help you with your projects. Our expertise allows us to provide students with high-quality academic writing, editing & proofreading services.
Free Features
Free revision policy
$10Free bibliography & reference
$8Free title page
$8Free formatting
$8How Our Essay Writing Service Works
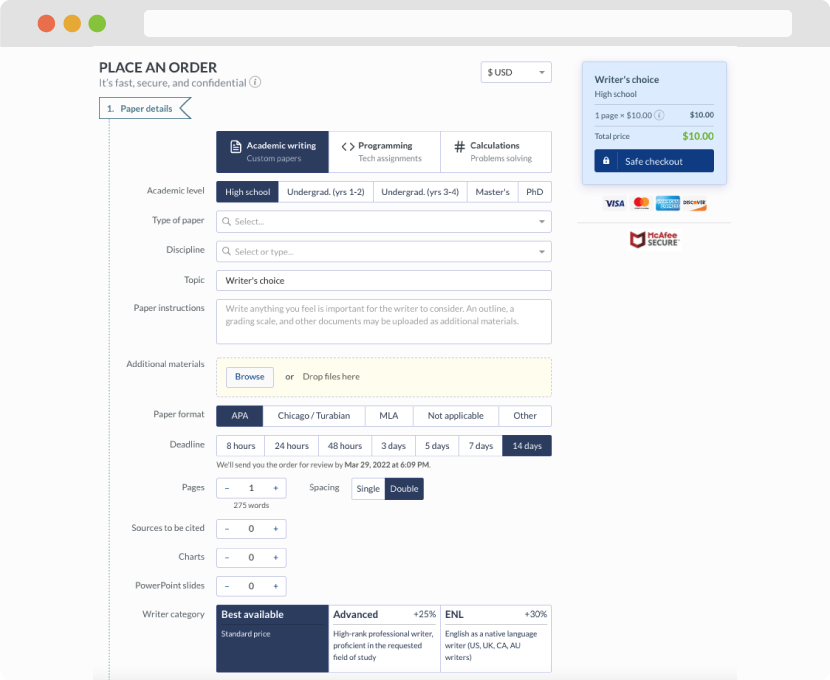
First, you will need to complete an order form. It's not difficult but, in case there is anything you find not to be clear, you may always call us so that we can guide you through it. On the order form, you will need to include some basic information concerning your order: subject, topic, number of pages, etc. We also encourage our clients to upload any relevant information or sources that will help.
Complete the order form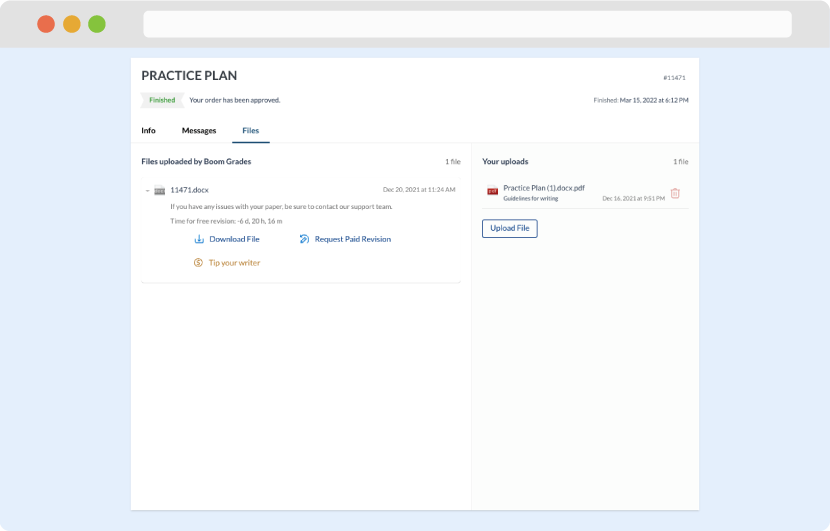
Once we have all the information and instructions that we need, we select the most suitable writer for your assignment. While everything seems to be clear, the writer, who has complete knowledge of the subject, may need clarification from you. It is at that point that you would receive a call or email from us.
Writer’s assignment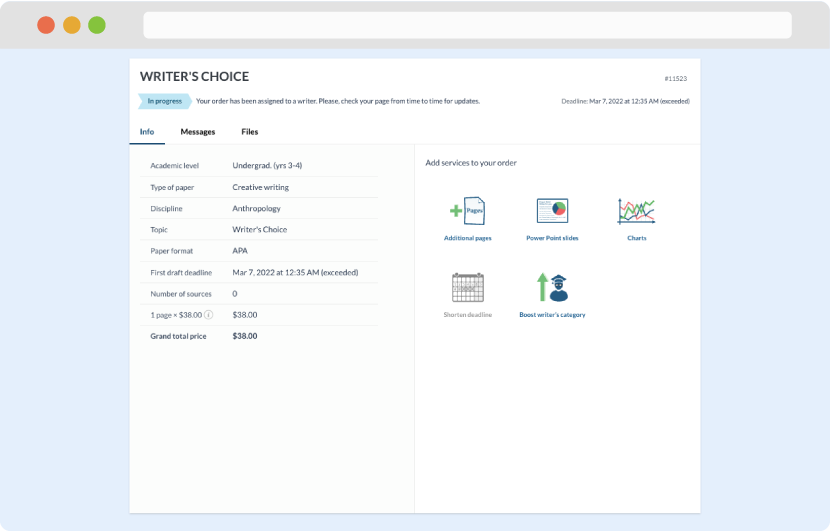
As soon as the writer has finished, it will be delivered both to the website and to your email address so that you will not miss it. If your deadline is close at hand, we will place a call to you to make sure that you receive the paper on time.
Completing the order and download